Previous exposure to the dengue virus may increase the potency of Zika infection, according to research from Imperial College London.
The early-stage laboratory findings, published in the journal Nature Immunology, suggests the recent explosive outbreak of Zika may have been driven in part by previous exposure to the dengue virus.
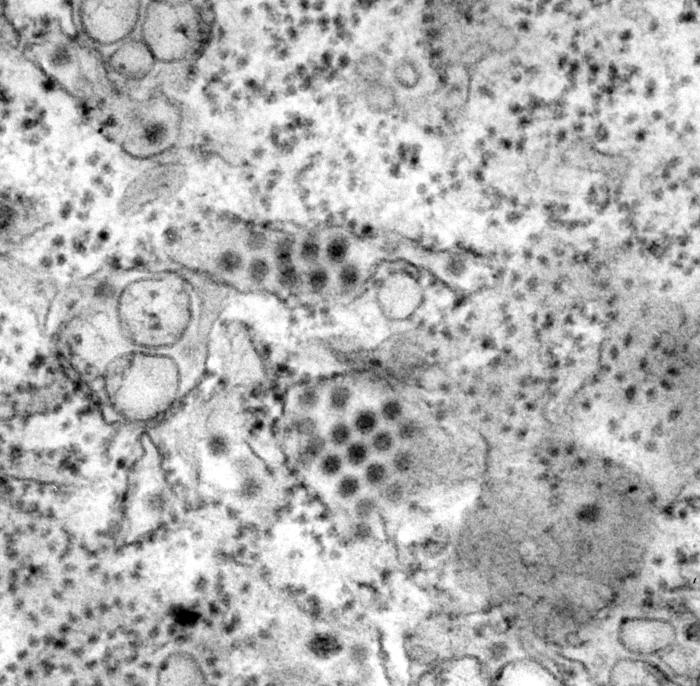
The study, which included scientists from Institut Pasteur in Paris and Mahidol University in Bangkok, suggests the Zika virus uses the body’s own defences as a ‘Trojan horse’, allowing it to enter a human cell undetected. Once inside the cell, it replicates rapidly.
Professor Gavin Screaton, senior author of the research and Dean of the Faculty of Medicine at Imperial, said: “Although this work is at a very early stage, it suggests previous exposure to dengue virus may enhance Zika infection. This may be why the current outbreak has been so severe, and why it has been in areas where dengue is prevalent. We now need further studies to confirm these findings, and to progress towards a vaccine.”
A second study by the same team, published in Nature, suggests an antibody that works against the dengue virus may also neutralise Zika – providing a potential target for a vaccine.
Dengue fever has risen dramatically over recent decades and the virus is thought to cause around 390 million infections each year – with 40 per cent of the world’s population living in areas of risk.
The dengue virus is similar to the Zika virus – they belong to the same viral family, called the Flaviviridae, and both are transmitted by the Aedes mosquito.
In the new Nature Immunology paper, supported by the Wellcome Trust and the Medical Research Council, the researchers used antibodies that recognise the dengue virus collected from individuals who had been infected with dengue. The team, who were also supported by the National Institute for Health Research Imperial Biomedical Research Centre, added them to human cell cultures, together with the Zika virus.
Their results suggest dengue antibodies can recognise and bind to Zika, due to the similarities between the viruses. Crucially, they also suggest that pre-existing dengue antibodies can amplify a Zika infection through a phenomenon called antibody-dependent enhancement (ADE).
This has been previously identified in dengue fever, and is thought to be why a second infection with dengue is often more serious than the first.
When dengue first infects the body, the immune system makes antibodies against the virus. Antibodies are large proteins that latch onto invading bacteria or viruses, neutralising them and enabling the immune system to destroy the pathogens. The antibodies are then primed to recognise the same invaders should another attack occur.
However, there are four different types of dengue virus. If someone is infected a second time by a different strain, the antibodies from the first attack can only partially bind to the virus, and are unable to prevent infection.
The antibody, with the virus loosely attached, then shuttles into an immune cell. This immune cell would normally then kill the virus, but because the virus is not properly attached, it breaks free once it gains entry to the human immune cell. Here it hijacks the immune cell’s machinery to replicate more viral particles, enhancing the infection.
The new study suggests the same phenomenon occurs when a person who has previously been exposed to dengue encounters Zika. The existing dengue antibodies latch onto Zika, due to similarity between the viruses. However the antibodies are unable to latch onto Zika securely, and so the antibody simply facilitates entry of Zika into the human immune cells, where it replicates.
“We now need to investigate whether the phenomenon of ADE may aid transfer of Zika across the placenta,” explained Dr Juthathip Mongkolsapaya, co-author from the Department of Medicine at Imperial.
She added that the team also found that a type of antibody may help protect against the phenomenon of ADE, and prevent the virus from hijacking the immune cells. Previous work from the team has shown the immune system generates different types of antibodies to dengue that bind to various areas of the virus. In the current study, the team found a group of antibodies that bind to a certain site on the dengue virus – called EDE1 antibodies – were able to prevent the Zika virus from entering the immune cell.
In a second study, published in Nature and co-authored by Professor Felix Rey from the Institut Pasteur and Professor Screaton from Imperial, the team confirmed that EDE1 antibodies bind efficiently to the Zika virus and potently neutralise infection. The team are now working hard to use these findings to develop new vaccines to dengue and Zika.
Dr Jeremy Farrar, Director of the Wellcome Trust, said: “Zika and dengue come from the same family of viruses and we know they share many similarities in their genetic make-up, transmission pattern and in the immune response they trigger. These new studies suggest that prior infection with dengue doesn’t offer any protection against Zika, and may in fact predispose people to a more severe infection. We can’t say yet whether this interaction is playing a role in the current outbreak, but if confirmed it’s likely to have important implications for the control and global spread of Zika, and for the development of any vaccine for the virus. There are still more questions than answers about Zika and this group of viruses including dengue. We know that Zika has been present in Southeast Asia and Africa for many years and yet has not taken off there as it has in South America. This is what the international research effort needs to work out, and quickly.”
Related:


One thought on “Dengue history may increase Zika potency: Study”