In a very rare occurrence, New York City health officials have reported a cluster of the bacterial infection, leptospirosis, that has affected three people within a one block section of the Concourse area of the Bronx during the the past two months.

All three cases had severe illness and were hospitalized with acute renal and hepatic failure. Two cases developed pulmonary hemorrhage and one died as a result of infection. The remaining two were discharged home.
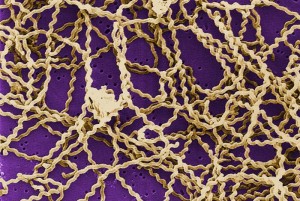
Leptospirosis is caused by a corkscrew-shaped bacterium called Leptospira interrogans, is often referred to as “rat fever” due to the principal role rats play in spreading the disease (scientists refer this type of animal as a reservoir host). Other animals can also be important reservoirs of the disease.
These animals can spread the disease in their urine, contaminating water, soil, or food. People who live in close contact with domestic animals or wildlife are at higher risk for getting the disease.
People become infected by coming into contact with contaminated urine, water, food, or soil through breaks in the skin, eyes, mouth, or nose. Outbreaks of leptospirosis are usually caused by exposure to contaminated water, such as floodwaters. Person to person transmission is rare. Infected individuals initially experience fever, severe headache and muscle aches, abdominal pain, and occasionally a skin rash. Patients in the later stages of disease can suffer from jaundice, kidney failure, bleeding from the mouth or nose, bloody urine and can be fatal, especially without proper treatment.
In New York City, most human cases are associated with exposure to rats, or rodent infested environments. Infected animals may excrete the bacteria into the environment.
During the past decade, NYC health officials have seen 26 leptospirosis cases from all five boroughs. This is the first time a cluster of cases has been identified.
Health department officials are reminding healthcare providers to consider leptospirosis in any patient presenting with evidence of acute renal and hepatic failure, or any patient with clinically compatible illness and a history of exposure to rats or environments contaminated by rat excreta. Leptospirosis can be treated with antibiotics.
Health officials offer the following recommendations to prevent leptospirosis:
- Avoid contact with rats or places where rats may have urinated.
- If you cannot avoid areas where rats have been seen, or if you are cleaning areas where rats have been, use a solution of one part household bleach and ten parts water to kill the leptospirosis bacteria.
- You can protect yourself from contact with rat urine by wearing rubber gloves, especially if you have cuts or sores on your hands or arms. You can also wear boots, masks and some type of eyewear.
- Wash your hands carefully with soap and water after any contact with areas where rats may live.
- Always wear shoes whenever taking trash to your trash compactor room.
Dogs are also susceptible to leptospirosis and you should ask your veterinarian if your dog needs to be vaccinated.
Related:
- Yellow fever vaccination update for travelers to Brazil
- Malaria, yellow fever and cholera outbreaks strain Angola’s health system
- Belize recognized for achievements in vaccination and malaria
- Victoria Health issues Ross River virus health advisory


One thought on “NYC: Leptospirosis cluster reported in the Bronx, one dead”