A case of anthrax in cattle was confirmed in the Dirranbandi-St George area in early July 2018. This detection is the fourth incident in cattle in the region since 2016.
Image/Biosecurity Qld
Animal owners in southern Queensland – particularly in the Dirranbandi to St George area – should be alert to anthrax and the risks to human and animal health. Vaccination of livestock can prevent unnecessary livestock deaths. Talk to your private veterinarian about anthrax vaccination.
Officials remind producers to adhere to the general biosecurity obligation (GBO) in preventing and managing incidents of anthrax.
In addition, in the case of an animal that died suddenly, officials say that producers contact a private veterinarian who can assist in determining the cause and provide biosecurity advice to protect human and animal health.
Anthrax: St George case prompts call to vaccinate livestock
Anthrax can infect humans (meaning there are additional considerations to be made to protect people), and incidents in livestock can have significant economic, environmental, and animal health and welfare impacts.
Anthrax typically presents as sudden death in livestock; can affect a wide variety of species (cattle, sheep, goats and camelids are particularly susceptible); often causes carcasses to bloat quickly; and may cause bloody or tarry discharges from carcass orifices.
It can affect one to two animals in small incidents, and exceed 100 animals in large outbreaks.
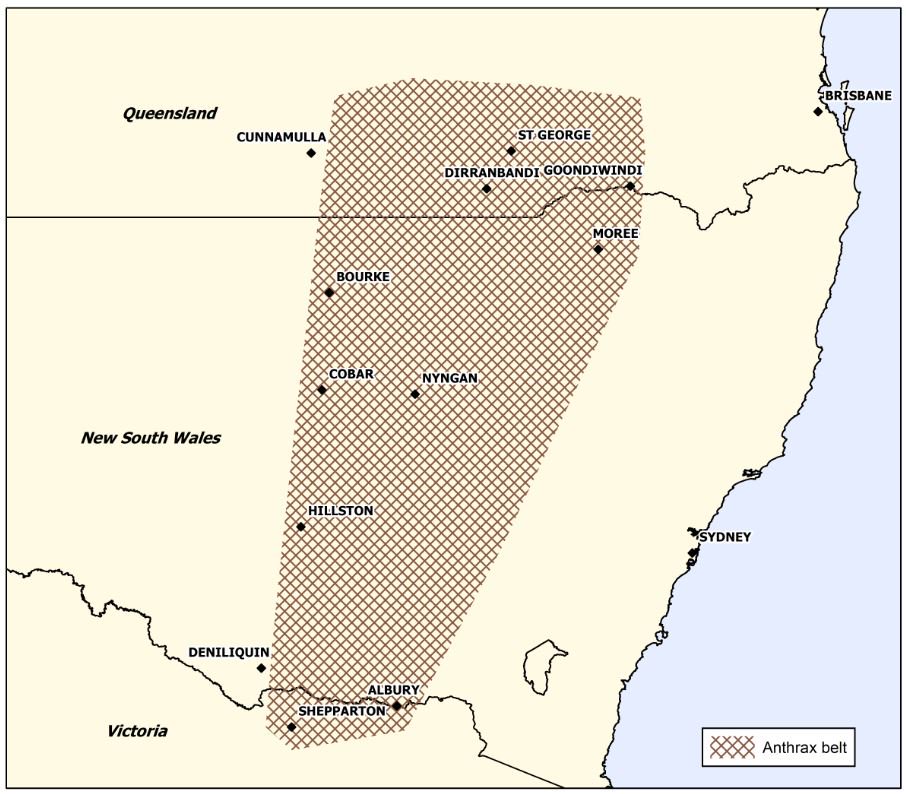
Soil that is contaminated with anthrax can be infective for decades (see map of the ‘anthrax belt’ below).
Management of an anthrax incident may include disposal, decontamination and vaccination.
- Parasitic infection, Strongyloidiasis, may be infecting up to 60 percent in remote northern Australia
- Australia: Increased reports of Buruli ulcer in Victoria
- Australia reports two gonorrhea ‘superbug’ cases: Alert issued
- Lyme disease in Australia: LDAA funding new patient focused pilot research study


