A broad spectrum antibiotic that could become the first of its kind to treat specific Gram negative and Gram positive infections as well as tularemia, a bioterrorism threat, will undergo the last steps in development with support from the U.S. Department of Health and Human Services’ Office of the Assistant Secretary for Preparedness and Response (ASPR).
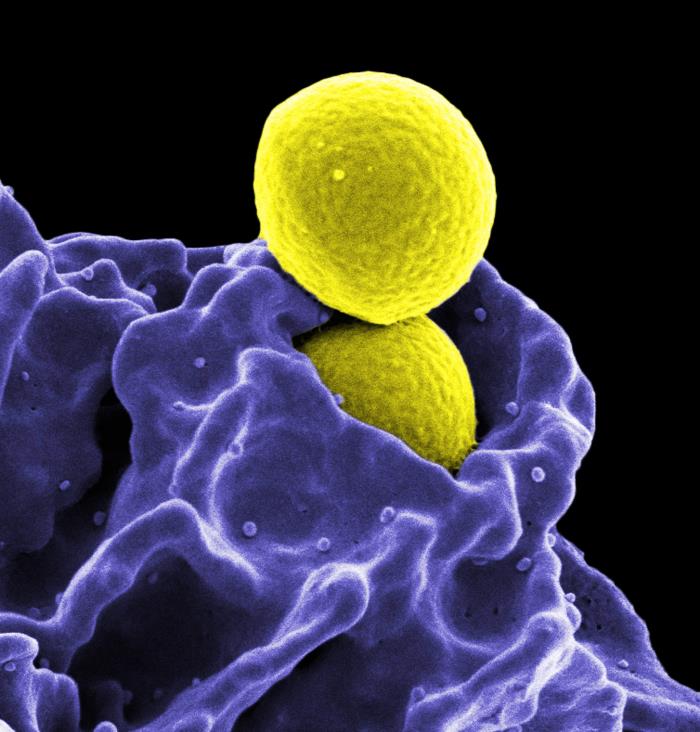
Image/NIAID
Under an 18-month, $20 million agreement between ASPR’s Biomedical Advanced Research and Development Authority (BARDA) and Basilea Pharmaceutica International Ltd, the company will conduct Phase 3 clinical studies of the antibiotic, Ceftobiprole, in treating specific Gram-negative and Gram-positive infections. BARDA has the option to extend the agreement for up to a total of four-and-a-half years and up to a total of approximately $100 million.
The Phase 3 studies are necessary to apply for U.S. Food and Drug Administration (FDA) approval. In addition, Basilea will evaluate Ceftobiprole’s potential as a treatment for tularemia, which can cause deadly pneumonia infections and could be used as an agent of bioterrorism.
Gram-negative and Gram-positive bacteria have different characteristics, often requiring different classes of antibiotics. Ceftobiprole is being developed as a potential treatment for skin infections, bloodstream infections and pneumonia including those caused by Methicillin-Susceptible and Methicillin-Resistant Staphylococcus aureus (MSSA and MRSA, respectively) as well as infections caused by the Gram-negative bacteria, such as Pseudomonas aeruginosa.
If approved by FDA, the drug could be marketed commercially for the treatment of these three infections and also could be available for use in a biodefense emergency. Ceftobiprole is the eighth broad-spectrum antimicrobial that BARDA has supported to date.
“HHS is working aggressively to address the nation’s needs in public health emergencies,” BARDA Acting Director Richard Hatchett, M.D., said. “Those needs include treatments for antibiotic-resistant bacteria and to strengthen our defense against bioterror threats; by identifying a number of products that can address both needs, BARDA’s biodefense investments will yield important public health dividends.”
Methicillin is an antibiotic that has long been used to treat Staphylococcus aureus infections. MRSA is resistant to methicillin and many other antibiotics. In the community, most MRSA or MSSA infections are skin infections, but in hospitalized patients these bacteria can cause deadly bloodstream infections, pneumonia and surgical site infections. MRSA infections also are associated with longer hospital stays, longer durations of antibiotic use, and higher treatment costs.
Pseudomonas aeruginosa can cause skin or ear infections after exposure to water, such as inadequately chlorinated swimming pools or hot tubs, or eye infections in people using extended-wear contact lenses. Serious, life-threatening Pseudomonas infections may occur in people with weakened immune systems and in hospitalized patients. More than 13 percent of healthcare-associated Pseudomonas infections each year are multidrug-resistant and result in hundreds of deaths annually.
Infections with MSSA, MRSA, or Pseudomonas aeruginosa occur more frequently in patients who have diabetes and can be life-threatening to hospitalized patients, particularly the elderly, and people with weakened immune systems.
CDC estimates that in the United States, more than two million people are sickened every year with antibiotic-resistant infections, with at least 23,000 dying as a result.
Related:

