An outbreak of monkeypox has affected 19 and killed seven people during the first two months of 2017 in Likouala province in northern Republic of the Congo, according to the Congo Ministry of Health and Population (MOHP).
The outbreak originated in Betou district on 16 January 2017 when the index case, a male hunter, developed illness. Subsequent cases emerged from three other districts between 27 January and 28 February 2017.
Two samples obtained from the suspected cases tested positive for monkeypox by PCR at the Institut National de Recherche Biomédicale (INRB), Kinshasa.
Monkeypox is a zoonotic disease indigenous to Central Africa. In humans, the disease is similar to smallpox, though milder. The current monkey pox outbreak in Congo is occurring in areas/districts that experienced similar outbreaks in 2010. The high CFR of 36.8% (7/19) is a cause for serious concern for public health.
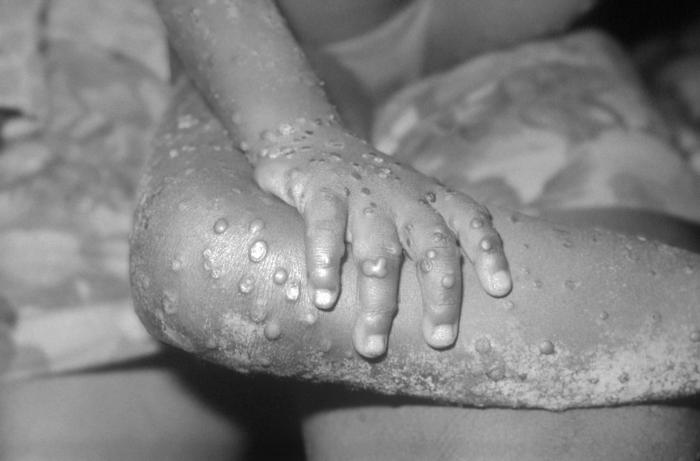
According to the CDC, the symptoms of monkeypox are as follows: About 12 days after people are infected with the virus, they will get a fever, headache, muscle aches, and backache; their lymph nodes will swell; and they will feel tired. One to 3 days (or longer) after the fever starts, they will get a rash. This rash develops into raised bumps filled with fluid and often starts on the face and spreads, but it can start on other parts of the body too. The bumps go through several stages before they get crusty, scab over, and fall off. The illness usually lasts for 2 to 4 weeks.
Rodents, such as rope squirrels, door mice and pouched rats, are the suspected reservoir hosts, with monkeys and humans as secondary, spill-over hosts.
People at risk for monkeypox are those who get bitten by an infected animal or if you have contact with the animal’s rash, blood or body fluids. It can also be transmitted person to person through respiratory or direct contact and contact with contaminated bedding or clothing.
There is no specific treatment for monkeypox.
Related:


Hey Robert – where did you find this information? You usually link to ur sources. Thanks!
Hi Melissa, Thanks for pointing that out. It has been rectified.
Robert