A new study from HealthPartners Institute and Centers for Disease Control and Prevention (CDC) showed that Tetanus, Diphtheria and Pertussis (Tdap) vaccination was not associated with an increased risk for microcephaly or other major birth defects.
The study was published in the Nov. 1, 2016 issue of the Journal of the American Medical Association (JAMA).
This retrospective study of 324,463 births compared the occurrence of birth defects, including microcephaly, in babies born to women who received Tdap during their pregnancy to those women who did not. The study’s results and findings expand upon what is known about maternal Tdap vaccination safety.
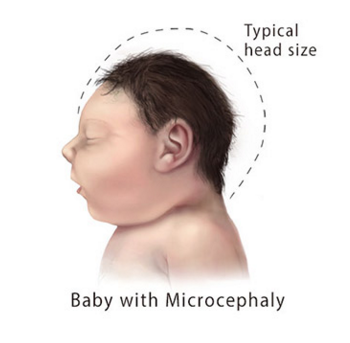
In 2012, the U.S. Advisory Committee on Immunization Practices recommended that Tdap vaccine be administered during every pregnancy, ideally between 27 and 36 weeks’ gestation. Previously, Tdap was recommended for unvaccinated pregnant women since 2010 in California and since 2011 across the United States. Cases of microcephaly (an abnormally small head due to failure of brain growth) in Brazil increased substantially during 2015, likely associated with maternal Zika virus infections. However, these cases overlapped with the November 2014 initiation of Brazil’s maternal Tdap program. Previous small observational studies reported no increased risks for birth defects following maternal Tdap vaccination; none focused on microcephaly.
In this study, Malini DeSilva, M.D., M.P.H., of HealthPartners Institute, Minneapolis, and colleagues included data from live births at 7 Vaccine Safety Datalink sites (Northern California, Southern California, Colorado, Minnesota, Oregon, Washington, and Wisconsin) from January 2007 through September 2013 and compared prevalence of structural birth defects between infants born to women who received Tdap during pregnancy and unvaccinated women. Analyses of maternal Tdap vaccination from 27 to 36 weeks’ gestation were limited to 2010-2013 for California sites and to 2012-2013 for other sites. Any structural defect, selected major structural defects, and microcephaly alone were identified from diagnostic codes assigned at medical visits during the first year of life.
The researchers found that maternal Tdap was not significantly associated with increased risk for microcephaly for vaccinations occurring at less than 14 weeks’ gestation (n = 3,321), between 27 and 36 weeks’ gestation (n = 20,568), or during any week of pregnancy (n = 41,654). Adjusted analyses were similar for any structural birth defect and selected major structural defects.
The authors note that the findings are potentially limited by incomplete data on Tdap vaccinations (making it possible to misclassify women’s immunization status), diagnosed structural birth defects, and important covariates (including maternal alcohol use), as well as inability to study birth defects resulting in pregnancy loss or elective termination.
“The findings support recommendations for routine Tdap administration during pregnancy,” the researchers write.


3 thoughts on “Tdap vaccine not linked to birth defects: Study”