Mosquito borne illnesses have become a concern in the United States once again in 1999 when West Nile virus was detected for the first time in humans here in New York City. Since that time, West Nile virus is a regular seasonal issue with a couple thousand deaths reported since 1999.
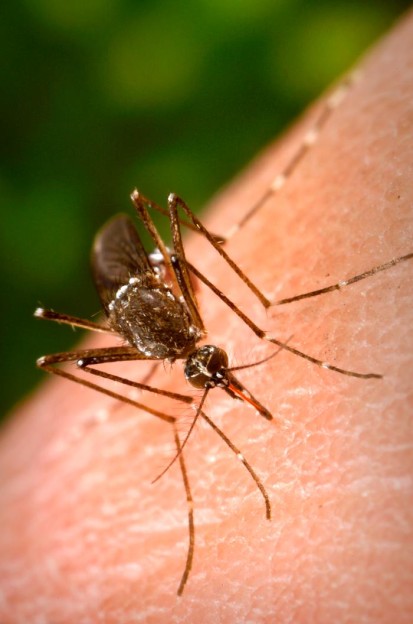
We also saw the emergence of chikungunya virus in the Western hemisphere in late 2013 and well over 2,000 travel associated and 11 locally acquired cases in this country.
To get a clearer picture on the state of West Nile virus (WNV), chikungunya (CHIKV) and the work of global environmental products and services company, Clarke, I had the opportunity to ask some questions to Dr. Rajeev Vaidyanathan, Director of Environmental Science at Clarke.
Robert Herriman: Let me start with chikungunya. Is this mosquito borne virus now here to stay in the US, like West Nile virus?
Dr. Rajeev Vaidyanathan: The transmission cycles, vectors, and hosts for CHIKV are different from those for WNV. First of all, CHIKV is not established in the U.S. like WNV. There are a few thousand cases of WNV every year, and since 1999 there have been over 41,000 clinical cases of WNV with almost 2,000 deaths. In comparison, almost 3,000 cases of CHIKV were reported in the U.S. in 2014, but these were acquired overseas. Only 11 cases of CHIKV were acquired locally – all in Florida.
Second, keep in mind that birds are the reservoir for WNV. While we don’t know what role birds or rodents might play as reservoirs in North America, at present humans seem to be the most important reservoirs for local CHIKV transmission. We have a better shot at controlling transmission of CHIKV in North America if the cycle is human-mosquito-human as opposed to bird-mosquito-human. Migrating birds with recrudescent (returning) infections can reintroduce a virus into a geographic area. On the other hand, humans are most infectious during the first 2-6 days of illness. That means a mosquito would have to bite a human during this early stage of infection, and a human infected the previous year is unlikely to act as a chronic reservoir of the virus the following spring and summer, when mosquitoes are biting.
Third, different mosquito species transmit WNV and CHIKV. That includes their feeding behavior and geographic distribution. The challenge of controlling Aedes mosquitoes is different – both of these species breed abundantly in and near human habitations. Both species will lay their eggs in the half inch of water that collects in a discarded candy wrapper and are thus highly successful in cities. We might expect to see more locally acquired CHIKV cases in our southern cities and suburbs where competent Aedes mosquitoes live among dense human populations.
RH: How far north is the Aedes mosquito vector found in the US?
RV: There are two species of Aedes mosquitoes that we know are competent vectors of CHIKV. Aedes aegypti is found throughout the southeast U.S. and as far north as Virginia, with established populations in Phoenix, Arizona, and Orange County, California. Aedes albopictus is common throughout the southeast and east coast, as far north as Pennsylvania, New Jersey, and southern New York and westward to Kansas, Oklahoma, and Texas. It has also been detected in parts of Arizona and New Mexico. We do not know the potential of other North American Aedes species to transmit CHIKV.
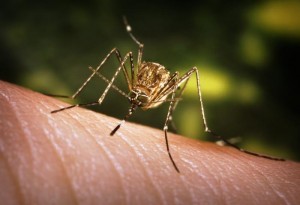
RH: Let me turn to West Nile virus, a virus transmitted by a different mosquito vector. So far this year, California is the state hit the hardest by WNV. Health officials blame it in part on the severe drought they are experiencing. How does drought affect the mosquito population?
RV: In years when there’s normal rainfall, the mosquito vectors of WNV have a lot of breeding sites where the females can lay their eggs. These are often open pools, or “dairy lagoons,” where animal waste accumulates. During times of drought, these natural and semi-natural water sources become depleted. Females then begin to lay eggs in water sources closer to human habitats like abandoned swimming pools, catch basins, and septic tanks. Drought also causes birds, which are the reservoirs of WNV, to come closer to human habitations to find food (grains, insects, worms). It’s this overlap of competent mosquito vectors for the virus and competent bird reservoirs for the virus near human habitations that lead to an increase in WNV transmission.
RH: Clarke specializes in preventing mosquito borne viruses here and abroad. Can you tell us about the techniques you use at Clarke in this work and about one success story using Clarke applications?
RV: An epidemiological response begins with surveillance, which takes two forms – larval or adult. We work closely with mosquito control districts (MCD) to conduct larval surveillance. There’s also adult trapping which gives us a sense of the flying population. We work with our partners to conduct surveillance and determine the location of breeding pools, so we can apply a larvicide in a preventive manner. Local MCDs conduct adulticiding applications to control adult mosquitoes. When mosquito populations reach a certain threshold, as determined by trap catches, MCDs start applying adulticides. Adulticide applications, either by ground or air, depend on the area that requires treatment – be they suburban homes, coastal areas, urban neighborhoods, or sites adjacent to wetlands.
The second step is attempting to control disease transmission. As a corollary to collecting mosquitoes, many districts also test mosquitoes and other animals, such as birds or rodents, for infectious agents. For example, districts in California might test dead crows for West Nile virus, and districts in Maryland might test chickens for eastern equine encephalitis virus. If MCDs just look at their mosquito counts and wait until the virus is detected in humans before controlling mosquitoes, they are responding too late. The number of infected mosquitoes has already exceeded a minimum threshold, and transmission to humans will continue unless MCDs take action. If districts are not collecting and testing mosquitoes from different habitats, then they are responding to outbreaks rather than anticipating them.
Three factors help a district decide to spray for mosquitoes:
- A mosquito population significantly greater than the baseline
- Isolations of virus from field collections of mosquitoes
- Isolations of virus from host animals
- Human cases.
If MCDs spray after human infections have been diagnosed, a fraction of the mosquito population is already infected. The best course of action is to spray at a certain population threshold or infection rate in mosquitoes. Even then, the very day of treatment, many people have been already bitten, and they are not going to show symptoms for another few weeks.
When we worked in Dallas in 2012, we were not a part of the surveillance phase. Up to the time they called us in to help, they were conducting their own program. Clarke was called to respond once warning signs were lit up. What triggered this was all these independent communities doing different things. If one controls their mosquito population, and the next doesn’t, the discrepancy will not have much effect in eliminating populations. Mosquitoes don’t recognize boundaries. They needed to treat a wider area with an aerial application. They kept doing these carve outs of communities who didn’t want to participate. We encouraged them to encompass the full area where they saw the breeding. When there is surveillance over a large metro area, it’s possible to pre-identify hot spots for mosquitoes, and then lay out their adulticide and larvacide appropriately. Pre-testing applications also is a huge factor in ensuring mosquito control. This includes testing as we make those applications to make sure we are getting droplets down of the correct size, pre and post trapping, so you know your populations prior and after treatment, and then ensure the populations are going down. You could have weather conditions to refuse if you weren’t anticipating properly. We do monitor that, and can see that data where he is there treatment where it immediately dropped off.
RH: If you were to look into your crystal ball, what do you see as the biggest mosquito-borne issue in the US, say in 3-5 years from now?
RV: I frequently ask district managers around the U.S. – what keeps you up at night? What do you worry about? Mosquito biologists and MCD directors agree that there are common threats:
- Insecticide resistance: There are a limited number of modes of action for adulticiding, killing adult mosquitoes, and there’s evidence of resistance in species in the US and globally. These concerns are a call to industry, one that Clarke is leading. We are developing and testing chemistries with new modes of action for resistance management.
- Invasive species: From 2013 to 2014, five records of mosquito species from Louisiana and Texas were found in Florida. Two species were found in Arizona and California that normally only occurred in the Southeastern United States and we also saw other species with international origins. “While we don’t know the potential of these species to spread in their new habitats, the effort to control them is substantial.” These species are transported from country to country inside tractor tires or inside pallets. Florida, Arizona and Southern California have breeding populations of species that had not been detected in those areas before 2013 and 2014. Some of these species are vectors of viruses. Their introduction and persistence in new regions changes how local MCDs must think about mosquito control. For example, in California, the two species from the Gulf Coast are container breeders; they breed in trash, tires, and flower pots around human homes. Mosquito control operators in California are accustomed to species that breed in stagnant rice fields or wastewater management systems. Because they have not had to contend with species that breed in and around homes, MCDs in California will need to adopt new strategies to control new, invasive species.
- Geographic spread of Dengue and Chikungunya viruses. The vectors of dengue and chikungunya viruses are common in the southeast and eastern U.S. Because the geographic range of these species is expanding, we might start seeing transmission of exotic viruses in other regions of the country, including California and Arizona.
Clarke is a global environmental products and services company dedicated to making communities around the world more livable, safe and comfortable.
Robert Herriman is a microbiologist and the Editor-in-Chief of Outbreak News Today
Follow @bactiman63


7 thoughts on “Chikungunya, West Nile virus and mosquito control in the US: A chat with Clarke’s Dr. Rajeev Vaidyanathan”