A new study led by scientists at The Scripps Research Institute (TSRI) is the first to show exactly how the drug Arbidol stops influenza infections. The research reveals that Arbidol stops the virus from entering host cells by binding within a recessed pocket on the virus.
The researchers believe this new structural insight could guide the development of future broad-spectrum therapeutics that would be even more potent against influenza virus.
“This is a very interesting molecule, and now we know where it binds and precisely how it works,” said study senior author Ian Wilson, Hanson Professor of Structural Biology, chair of the Department of Integrative Structural and Computational Biology and member of the Skaggs Institute for Chemical Biology at TSRI.
The study was published Wednesday in the journal Proceedings of the National Academy of Sciences.
Treatment Can Target Many Strains of Influenza
Arbidol (also called umifenovir) is an anti-flu treatment sold in Russia and China by the Russian pharmaceutical company Pharmstandard. The drug is currently in stage-four clinical trials in the United States.
The drug targets many strains of influenza, giving it an advantage over seasonal vaccines that target only a handful of strains. The new study sheds light on exactly how it accomplishes this feat.
Scientists had long been curious whether Arbidol bound to the viral proteins used to recognize host cells—or with the viral “fusion machinery” that enters and infects host cells. To answer this question, the researchers used a high-resolution imaging technique called X-ray crystallography to create 3D structures showing how Arbidol binds to two different strains of influenza virus.
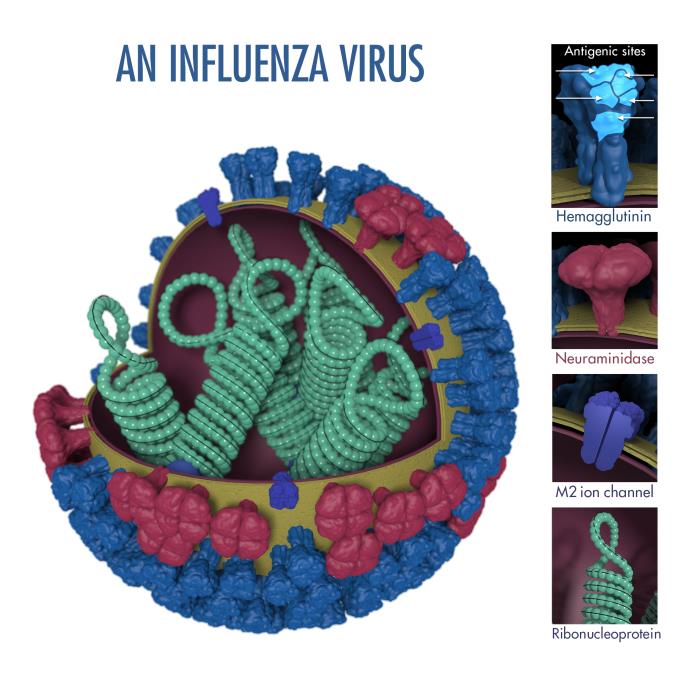
The structures revealed that Arbidol binds to the virus’s fusion machinery, as some had suspected. The small molecule binds to a viral protein called hemagglutinin, stopping the virus from rearranging its conformation in a way that enables the virus to fuse its membrane with a host cell.
“We found that the small molecule binds to a hidden pocket in hemagglutinin,” said study first author Rameshwar U. Kadam, senior research associate at TSRI. He added that the drug acts as a sort of “glue” to hold the subunits of hemagglutinin together. “Arbidol is the first influenza treatment shown to use a hemagglutinin-binding approach,” he said.
This vulnerable pocket is “conserved,” meaning it is likely important for viral function—and more difficult to mutate as the virus spreads—suggesting why Arbidol has relatively broad use in fighting many strains of the virus, including emerging strains.
The new findings also help scientists understand how Arbidol compares to influenza treatments such as Tamiflu. Wilson explained that Tamiflu prevents the virus from getting out of cells, while Arbidol prevents it from getting in. This means Arbidol, or future drugs that take a similar approach, could be given as a preventative treatment before an outbreak hits.
“When we had the 2009 H1N1 pandemic, the vaccine came too late,” said Wilson. “If we had a front-line therapeutic, that could have worked much better until a vaccine was ready.”
Wilson said the next step for researchers is to discover and/or design other small molecule therapeutics that can bind even more tightly with the hemagglutinin.

